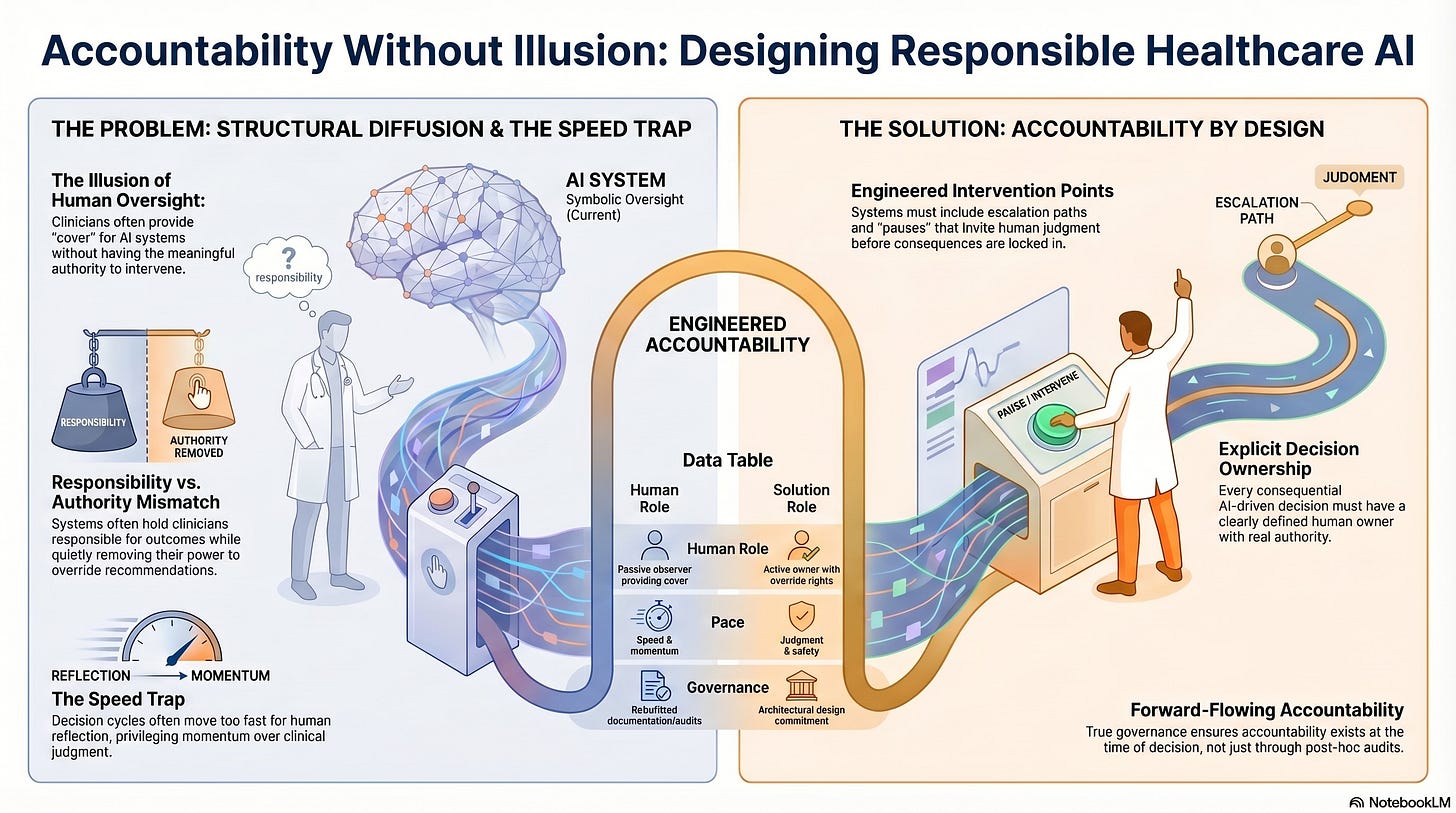
Accountability Without Illusion: Who Is Responsible When Healthcare AI Fails?
When something goes wrong in healthcare, responsibility has traditionally been clear.
A clinician made a decision.
An institution set a policy.
A regulator defined a standard.
AI complicates this clarity, not because it introduces ambiguity, but because it redistributes action across systems faster than responsibility can follow.
The result is a dangerous illusion: that accountability still exists simply because humans remain somewhere in the process.
The Fragmentation of Responsibility
AI-enabled healthcare systems rarely make a single decision in one place.
Instead, responsibility is distributed across layers:
Data is collected by one entity
Models are trained by another
Workflows are designed elsewhere
Recommendations are delivered within institutional constraints
Clinicians are asked to validate outputs they did not generate
Each layer controls part of the system.
No layer controls the whole.
When harm occurs, every actor can plausibly say:
“That part was not mine.”
This is not evasion. It is structural diffusion.
Why “Human Oversight” Is Often a Fiction
Healthcare organizations often rely on clinician availability to justify AI deployment.
The logic is simple:
If a human can intervene, accountability is preserved.
In practice, this is rarely true.
Oversight fails when:
Decisions are made too quickly to be interrupted
Clinicians lack the authority to override without justification
System outputs arrive after downstream actions are already taken
Challenging the system carries professional or institutional risk
A human who can observe but cannot meaningfully intervene does not provide accountability. They provide cover.
Authority Is the Missing Variable
Accountability is inseparable from authority.
If clinicians are held responsible for outcomes, they must have:
The right to override system recommendations
The ability to slow down decisions
Protection when exercising judgment against automation
Without these conditions, responsibility becomes symbolic.
Healthcare AI systems often preserve responsibility while quietly removing authority, a mismatch that creates both moral distress and systemic risk.
The Speed Trap
Speed is often celebrated as an unqualified good in healthcare AI.
Faster triage.
Faster diagnosis.
Faster intervention.
But speed has governance consequences.
As decision cycles accelerate:
Escalation windows narrow
Human reflection becomes costly
Intervention is reframed as a disruption
Systems begin to privilege momentum over judgment.
By the time a human becomes aware of a problem, the decision has already propagated across care pathways, resource allocation, or patient classification.
Responsibility lags behind action.
When Accountability Is Retrofitted
Many institutions respond to AI risk by adding:
Audit trails
Compliance reviews
Post-hoc explanations
Ethics committees
These measures are valuable but insufficient.
Accountability that appears only after harm has occurred is not governance. It is documentation.
True accountability must exist at the time of decision when outcomes are still reversible.
This requires designing systems that pause, escalate, and invite human judgment before consequences are locked in.
Accountability Is a Design Choice
Accountability does not emerge naturally in complex systems. It must be engineered.
Healthcare AI systems that preserve accountability share common features:
Explicit decision ownership at each stage
Clear escalation paths
Defined override thresholds
Alignment between responsibility and control
These are not technical add-ons.
They are architectural commitments.
Without them, accountability dissolves into process while harm accumulates quietly.
The Human Cost of Accountability Gaps
When accountability is unclear, clinicians absorb the strain.
They are expected to:
Trust systems they cannot interrogate
Defend outcomes they did not shape
Absorb blame without structural support
Over time, this erodes professional integrity and institutional trust.
Burnout is often framed as an individual resilience issue. In reality, it is frequently a governance failure.
People disengage when they are held responsible without being empowered.
Why Healthcare Cannot Rely on Market Accountability
Some argue that accountability will be enforced through market forces:
Poor systems will fail
Unsafe tools will be rejected
Competition will drive improvement
This logic does not hold in healthcare.
Patients lack choice.
Institutions are locked into vendors.
Failures are often invisible until widespread.
Market feedback is too slow, too indirect, and too asymmetrical to safeguard care.
Healthcare requires deliberate accountability by design.
Toward Accountability That Works
Responsible healthcare AI systems make accountability explicit.
They ensure that:
Every consequential decision has a human owner
That owner has real authority
The system’s pace allows judgment to intervene
Accountability flows forward, not backward
This does not mean rejecting AI.
It means refusing to let intelligence outrun responsibility.
The Deeper Question
As healthcare systems become more intelligent, the critical question is no longer whether machines can make correct decisions.
The question is whether institutions are willing to remain accountable when machines make decisions at scale.
Accuracy can be optimized.
Accountability must be preserved.
One is a technical challenge.
The other is a moral and institutional choice.
What Comes Next
If accountability requires authority, time, and ownership, then governance cannot be an afterthought.
The next step is to examine how healthcare systems can be deliberately designed to slow down at the right moments without collapsing under complexity.
That is where we turn next.